Five billion. That’s the number of people in the world who have no access to basic surgical care according to the Lancet Commission Report on Global Surgery. Historically, the Western medical community tried to address this disparity with surgical mission work, where professionals would fly in, deliver care, and then depart.

In recent years, however, the limitations of this model have become clear. While mission work provides important care to patients, it doesn’t address the root causes of the lack of local surgical care.
In an effort to create long-lasting change, a new model of global surgery focuses on building local surgical capacity and sustainability. Several of our faculty are leaders in this movement, and we’re proud to engage in collaborative initiatives to expand surgical access across the world.
Building capacity, collaboratively
Addressing the global lack of surgical care requires integrating surgical services across all levels of care. Surgical capacity is determined by a number of factors, all of which improve infrastructure and training. It’s key that procedures are safe, affordable, and accessible, and that they are driven by local healthcare providers.
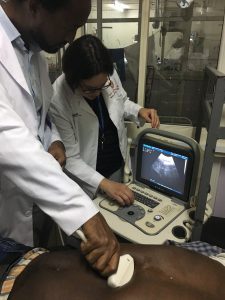
“The most important thing about global surgery is that it has to sustainable,” endocrine surgeon, faculty member, and global surgery researcher Dr. Kristin Long said. “It’s not a sustainable thing for US surgeons to travel for a couple of weeks a year, do some surgery, and then leave. What’s feasible is to educate the local providers, and make sure that they can perform this surgery safely.”
A key component of surgical capacity building is developing collaborative relationships with local partners. In a variety of partnerships across the world, our faculty have built strong connections with local surgeons and institutions. Our faculty provide training and support, helping local organizations grow so they can meet surgical demand.
Learning as much as we teach
Not only does working on surgical capacity provide education for local providers, but it also is an important learning opportunity for the US trainees who participate in these trips.
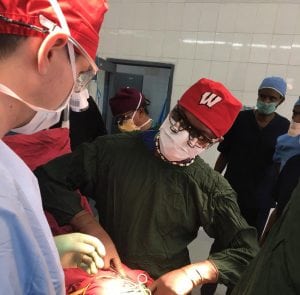
“I’ve learned just as much from the local providers,” endocrine surgery fellowship graduate Dr. Alexandra McDow said, describing her experience teaching endocrine surgery techniques in Kenya. “And I hope they’ve learned a lot from me as well.”
For trainees, performing surgery in unfamiliar environments is a valuable learning experience. Not only does this prepare them for future global surgery service, but it also prepares residents who are training for careers in rural surgery in the United States, where they may face a similar lack of equipment, or encounter diseases that would be treated by a specialist in a more populated area.
“You’re not always going to have every piece of equipment available to you, so to bring my trainees over here to see that reality and to experience it is very valuable to their education,” said Dr. Long.
Capacity building in Ethiopia

In addition to collaborating with global partners, we’re proud to partner with other US institutions. Dr. Girma Tefera is the Medical Director for Operation Giving Back, a program of the American College of Surgeons. He is the co-leader of their new pilot program collaborative, where 13 surgical departments are establishing a centralized surgical training hub at Hawassa University in Ethiopia. This collaborative program creates a year-round presence of US faculty and trainees to deliver higher quality surgical education, increase the number of local trainees, and reduce duplicative efforts.
“Hawassa is an excellent choice for piloting this program, as it is a relatively large teaching institution with a wide-ranging resident training model in place,” Dr. Tefera said. “The potential impact of this surgical training collaborative hub is extraordinary.”
The pilot program began last January and concluded in July 2019. As part of the pilot, Dr. Long and fellow faculty member Dr. Angela Ingraham traveled to Hawassa for a two-week rotation to assess local needs. For the next phase, each university will send 1-2 faculty members and residents for a month-long rotation. In May 2020, Dr. Long and Dr. Ingraham will return to Hawassa, accompanied by 1-2 general surgery residents.
We are proud to partner with programs like these to help bring surgery to the world.
“Most of us who do this would love to work ourselves out of a job, because if the local surgeons are capable of doing these surgeries, then they don’t need us, and that’s the ultimate long-term goal,” said Dr. Long.
Learn how you can support our global surgery and education work >>